Massage therapists live in a world of touch. So it is no surprise that the new science that relates to how touch, sensation and pain is processed and experienced would be relevant to massage therapists. This is particularly true since many clients seek out massage therapy for complaints specifically relating to pain.
Pain science in one form or another, has been around for years. One of our first understandings of it was provided by Descartes [1], who theorized that pain and physical illness were limited to a nervous system experience, i.e. you hurt your hand and so you feel it. It essentially separated the mind and body experiences.
As our understanding of pain sensation grew, we realized that feeling things was a far more complex process, and that our bodies are filled with different kinds of receptors that relay information, not just one way to process. Melzack and Wall changed [2] our perception further by bringing in the “gait control” theory to our clinical understanding. In this view, when the system is stimulated, it is sent through a ‘gait’ in the dorsal horn of the spinal cord. That gait however can be modulated by some psychological components resulting in a difference in the perception of the stimulus.
Our most current and newest understanding of pain is that of the biosocial understanding of pain. [3] In this model, we have a stimulus of some kind that is relayed to be processed, but at that point many factors such as environmental, social or emotional, might come into play to determine if pain is generated and at what intensity. And from that we see pain as an output of the brain, rather than something that is the result of poor biomechanics or even, in some cases, injury. In other words, pain can stand on its own without us having to find causation in the body.
What does this mean for Massage Therapy?
For a lot of massage therapists, this has left them a little confused as to their role in treatment. If pain is not generated exclusively in the body, what are we treating? If I am not ‘fixing’ a structure or posture, what am I doing? If pain is an output, then why seek physical treatment at all? It could be easy to start feeling a little redundant in the mix of it all, but now more than ever, massage is a viable option to those experiencing pain.
From a massage therapy perspective, the biosocial model of pain is far more inclusive than exclusive. If pain is influenced by thoughts, feelings and emotions, then doing things that feel good have the potential to benefit the client, even from a general treatment perspective. Asking your client “how do you feel?” during treatments and “was that good for you?” afterward becomes a relevant way to guide success for generalized treatment. It’s a step towards the clinical world seeing ‘feeling good’ as a part of heath care, rather than a luxury associated with indulgence. If the body is spending much of its time protecting us by sensing threats around us, we can also help send the message back to the body, that everything is “a ok” (within reason).
Don’t throw the baby out with the bathwater
It would be easy to read the new information coming out about pain and assume that from here going forward, massage has only general feel good treatments to offer in the context. Should massage therapists stop treating for specific conditions? The answer is both yes and no. Moving forward with quality treatments is going to have to do with how humble and honest a massage therapist can be with him or herself. And that is no easy task in an industry trying to prove itself as medical professional. Massage therapists have to accept two truths about their treatments and understand of them. 1. that they have a limited understanding and education about what they know about the person on their table. 2. That they may never know the answer to why the body has decided to protect itself.
This model does not mean that structural problems don’t exist. The normal rules of physics involving force, friction, leverage and space are still in effect. Bones still break, posture still degrades to bone-to-bone contact, and fitness plans still ramp up too fast, but a therapist has to be willing to open the door to other possibilities when the evidence does not add up, question it, even when it does, and treat the structural issue as a symptom rather than a cause in some cases.
Pitfalls in Treating Pain with Massage
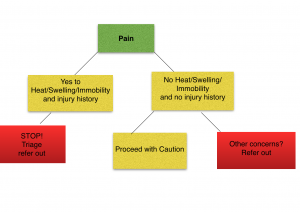
You may find yourself getting caught in a few traps if your a massage therapist treating people with pain. Operating safely in the biosocial model of pain does have its challenges. If pain is not always associated with injury, then assessing “pain” as a contraindication for treatment may not be the best guide. Without fail, a massage therapist must be able to assess the signs and symptoms of pain associated with acute injury pain-vs-the signs and symptoms of pain itself. The signs may not always be so clear. If you are inexperienced, it is always best to refer out so that you can remain safely in the boundaries of “Do No Harm”. A biosocial pain assessment for a massage therapist looks like this:
The sooner therapists get comfortable with treating pain, the sooner they can help get their clients comfortable. Next time we will go over the guidelines for talking to your clients about pain to provide some answers about when and how talking to people about their pain is appropriate in the contexts of Massage therapy as health care.
[1][2]R.Melzack, P.Wall. Science, New series, Vol. 150, NO. 3699.Nov, 19 1956 Pain Mechanisms: A new theory
[3] R.J. Gatchel, Psychological Bulletin, Vol. 133, NO 4, 581-624 2007. The Biopsychosocial approach to chronic pain: Scientific advances and future directions.
[wpseo_address oneline=”1″ show_state=”0″ show_email=”0″]