Learn how massage can improve your life
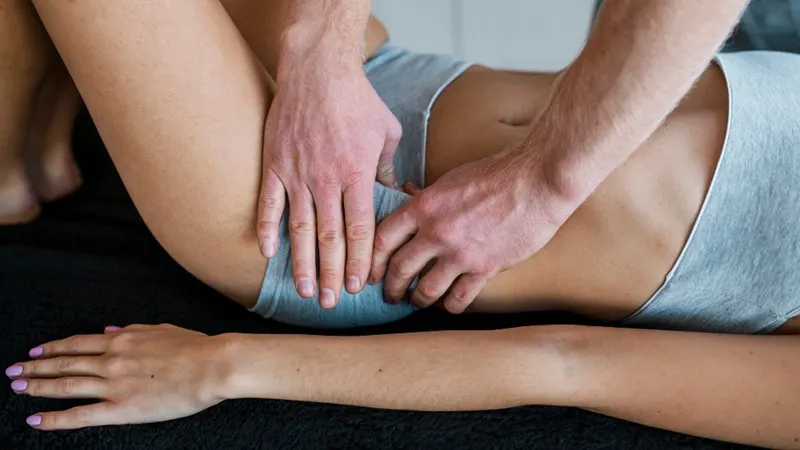
Should You Get a Massage Before Your Marathon or Race? You’ve put in the work. The long runs are behind you, your mileage is dropping, and race day is right around the corner. This is the part where things are supposed to feel easier—but in our experience, this is where a lot of runners start […]
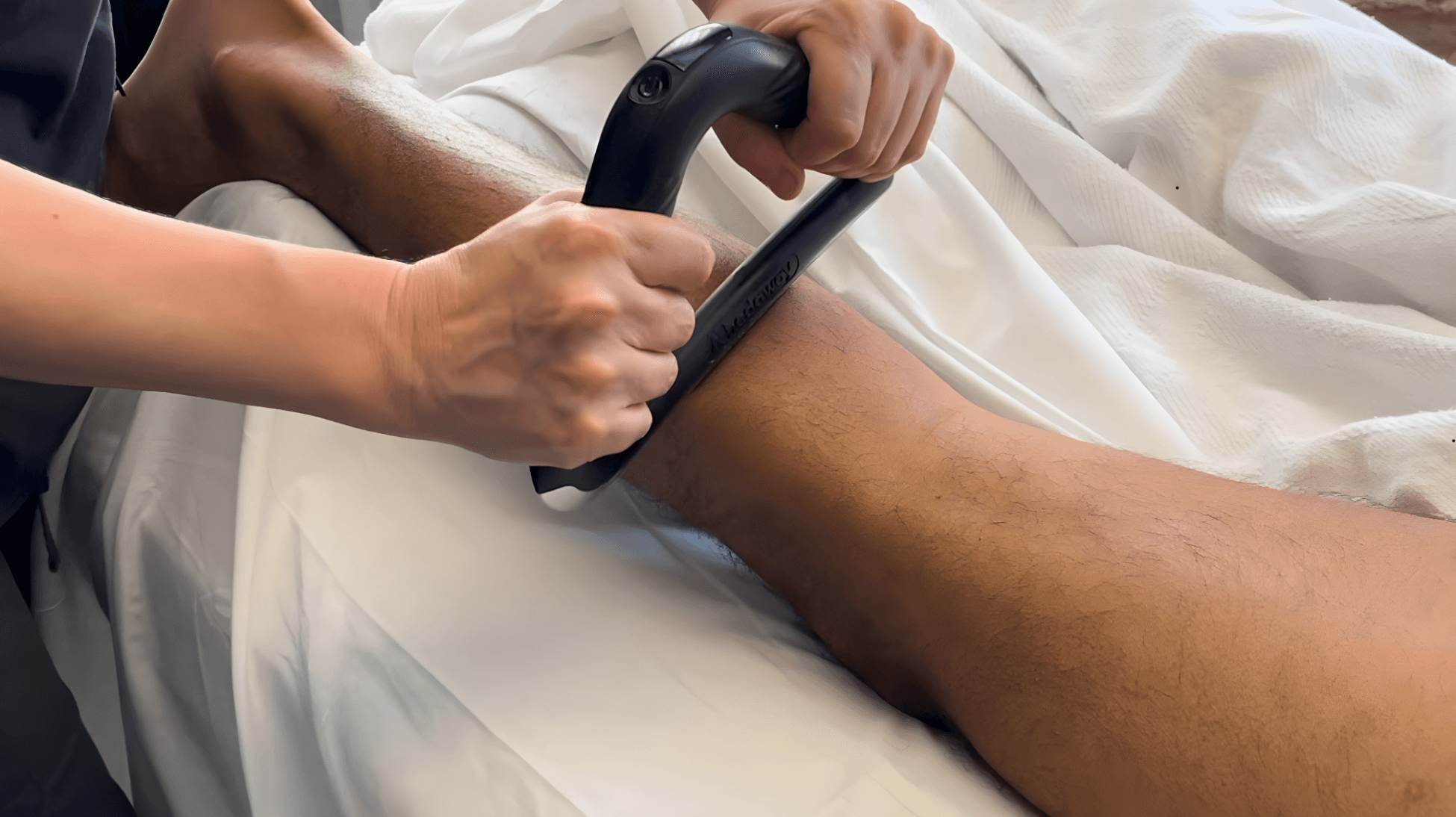
What Is a Massage Modality? Why It Matters for Your Massage Results When you book a massage, you might hear your therapist or the website mention different “modalities” used during your session. But what does a massage modality mean? Booking a massage and getting the results you want out of it can be super confusing […]

Mindful Ways to Reset Spring Break Style, When You’re Not Leaving NYC It’s that time of year, especially if you have kids—your feed is full of beach photos, family trips, and “out of office” replies, while you’re still at work, juggling responsibilities, and wondering when your break is coming. When it feels like everyone else […]

We think fall is the perfect time to get a massage, and here is why! As the leaves turn vibrant shades of red and orange and the air becomes crisp and cool, fall ushers in a season of change and transformation. Fall is the perfect time to get a massage. It’s also the perfect […]
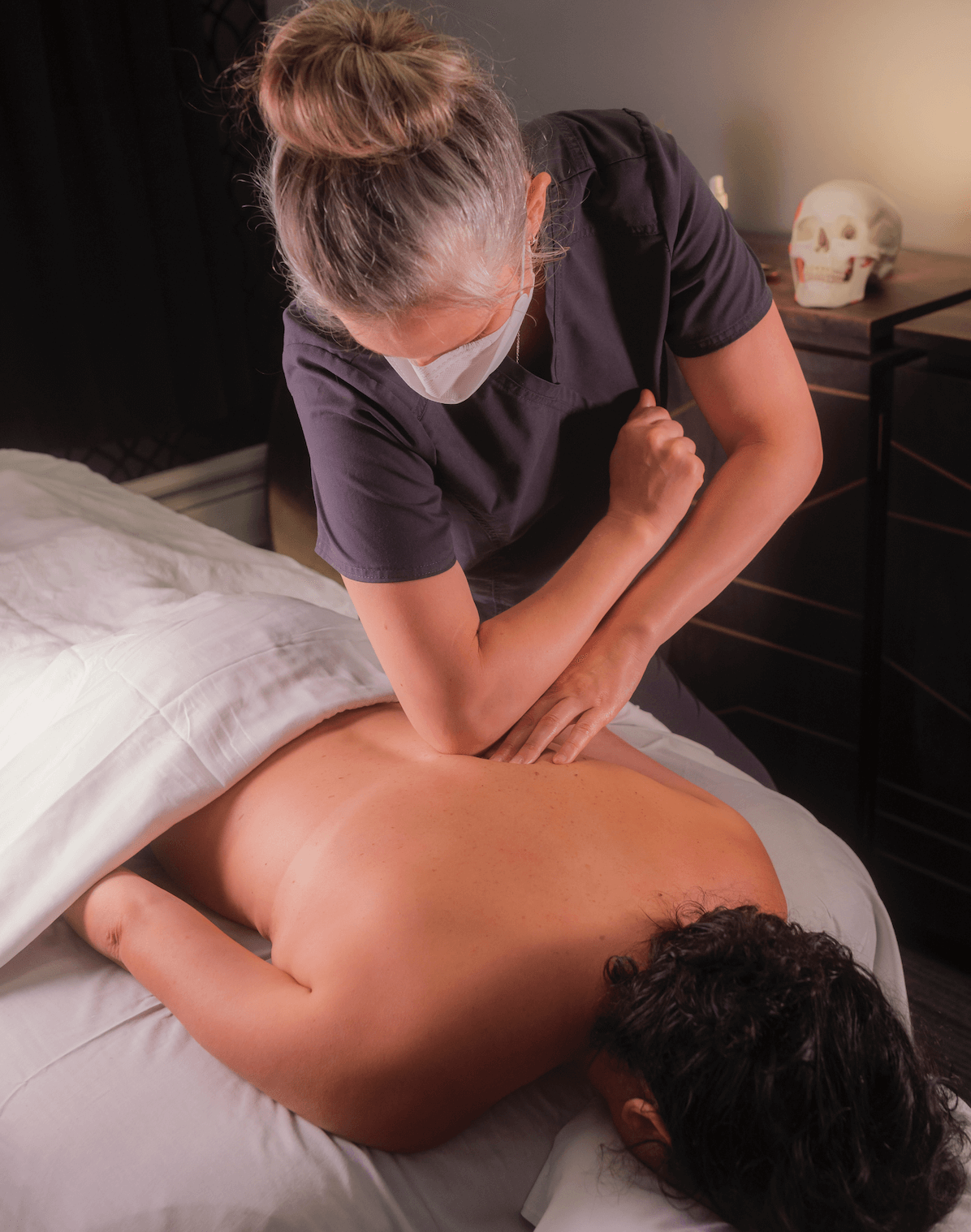
Massage or a Rub? We thought it might be a good idea to do a little post on the difference between a massage and a rub. Often these two things are confused, used interchangeably and the general public might not know that there is a difference. As a massage therapist, there is definitely a difference. […]
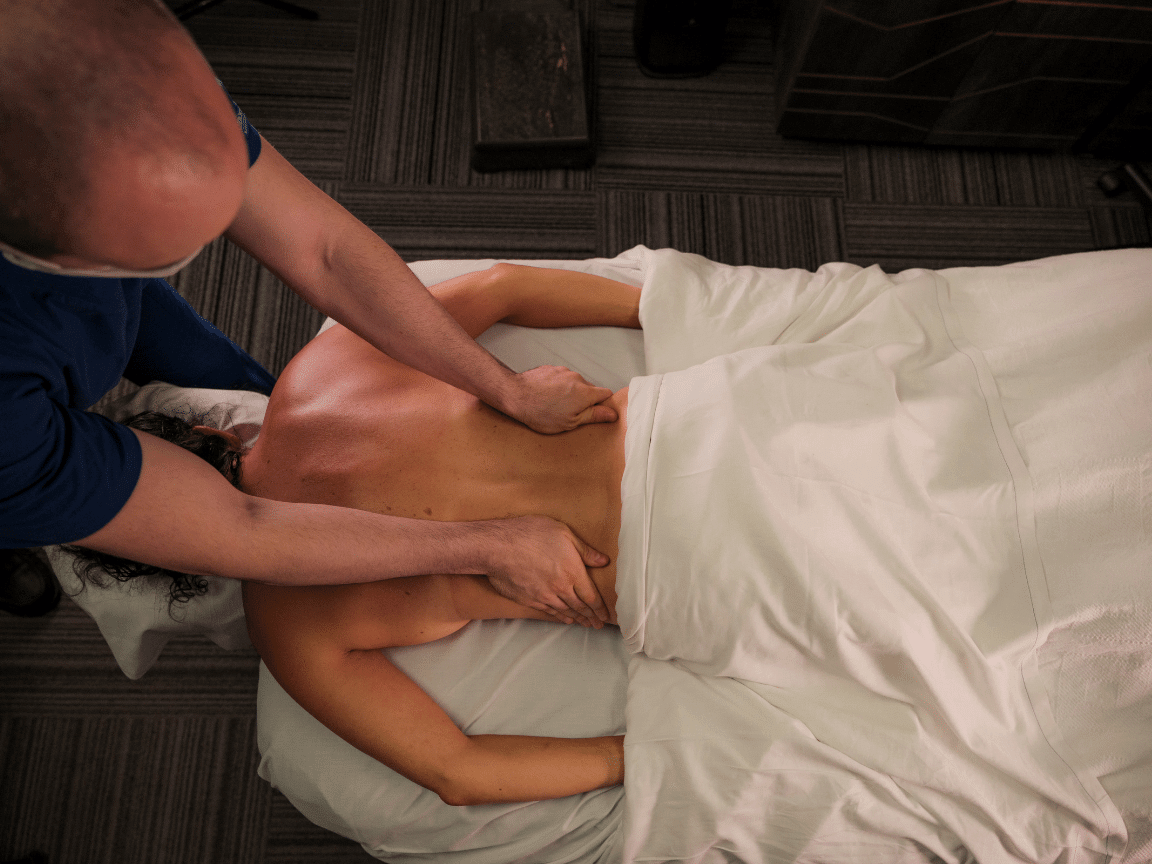
Introduction to back pain Low back pain is surprisingly common among all Americans and is one of the foremost reasons we miss work. Based on that it is not surprising that we are always looking for ways to solve, treat, or rid ourselves of nagging back pain. The truth is though, our medical system is […]

We welcome Medical Massage Therapist Erika to the Body Mechanics team! She gave us some insights into her life, passions and hobbies. Take a read to get to know her a little better!
Can Massage Therapy Help My Lower Back Pain? Can massage therapy help my pain? The answer to this question is more complicated than you would think. Massage Therapy research is all over the map. For starters, there are some inherent conflicts with the studies because people LIKE massages. And people are more likely to choose […]
Body Mechanics welcomes new Sports Massage Therapist Emanuel to the team! With experience in martial arts, sports, and training, Emanuel has many sources of knowledge to pull from when taking on a client! We spoke with him to get to know him a little better. What is your background in sports? Do you train? Participate? […]

Welcome to your local Massage Therapy information page for Body Mechanics Orthopedic Massage! If you are reading this blog, you probably have some questions about whether or not it is safe to receive a massage in the time of Covid-19, and what our practice and our cleaning regimen looks like since opening. If you have […]